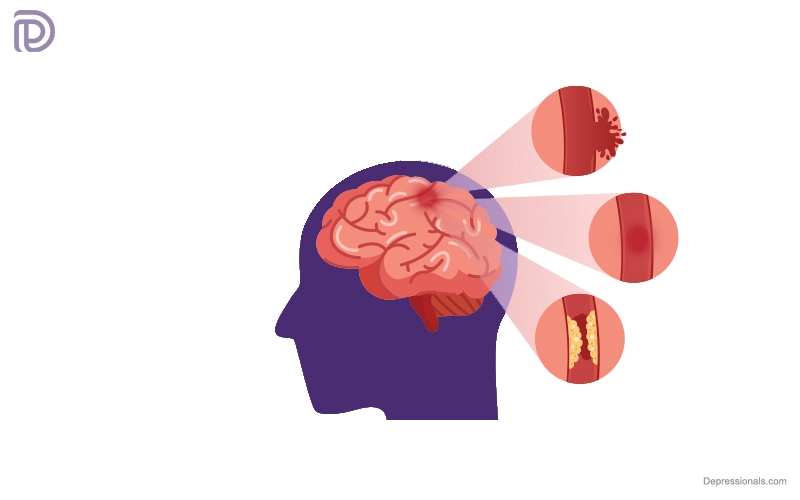
What is vascular dementia?
The second most common type of dementia is vascular dementia after Alzheimer’s disease. It occurs when the brain’s blood flow is reduced. It is possible for blood clots to completely or partially block the flow of blood to brain tissues.
A stroke or major surgery, like heart bypass surgery or abdominal surgery, can cause vascular dementia symptoms to surface gradually.
It’s hard to tell dementia and other similar conditions apart because they have similar symptoms. Blood flow problems to the brain cause vascular dementia, but they can happen in many different ways. Here are a few things you should know about vascular dementia:
- Mixed dementia: When Alzheimer’s and vascular dementia are present, this type is called mixed dementia.
- Multi-infarct dementia: The process occurs when a number of small, often “quiet”, blockages restrict blood flow to a specific area of the brain. Over time, the cumulative effect starts causing impairment symptoms even if the individual effects aren’t obvious at the time. Vascular cognitive impairment is also called multi-infarct dementia.
When the blood flow is reduced or stopped, the brain suffers depending on where and how much the affected area is. It doesn’t necessarily change the ability to carry on normal activities, though, if you have a small area of the brain that controls memory affected. Your ability to think clearly or solve problems or even your memory might vary if a larger area is affected.
The following factors will increase the risk of disorder in the coming decades:
- Vascular dementia is often caused by conditions that occur most commonly in older people, such as atherosclerosis (hardening of the arteries), heart disease and stroke.
- The average age of people over 65 is rising.
- Chronic diseases such as diabetes and heart disease are more common among older people.
Read: Chronic Fatigue Syndrome
What causes vascular dementia?
It is due to an insufficient supply of blood to a part of the brain that vascular dementia occurs. There are several factors that can reduce or stop blood flow to the brain.
- Blood clots
- Blood is lost when a blood vessel ruptures (e.g., after a stroke)
- Atherosclerosis, infection, high blood pressure, or an autoimmune disorder can damage a blood vessel
CADASIL is a form of dementia that is caused by a genetic disorder that results in subcortical cerebral infarctions and leukoencephalopathy. A parent who possesses the CADASIL gene passes it down to their children, meaning that this is an autosomal-dominant syndrome. Symptoms originate in the brain’s white matter and involve blood vessels. People often start having symptoms like migraine headaches, seizures, and severe depression in their mid-30s; however, they might not show up till later.
Who is at risk for vascular dementia?
Cardiovascular diseases, strokes, diabetes, and atherosclerosis rise to the top of the list of risk factors for vascular dementia:
- Increasing age
- High blood pressure
- Cigarette smoking
- High cholesterol and triglyceride levels
- Diabetes
- Fibrillation in the upper chambers of the heart (a fast, irregular beat)
- Homocysteine in the blood causes blood vessels to damage, cause heart attacks, and cause blood clots
- Not enough exercise
- Overweight or obesity
- Oral birth control pills
- Blood thickening or clotting conditions
- Dementia in family history
- Family history of CADASIL
Read: Frontotemporal Dementia
What are the symptoms of vascular dementia?
Vascular dementia symptoms manifests differently depending on where and how much brain tissue is affected. There may be a sudden or gradual onset of cerebral vascular dementia symptoms after a stroke. Other strokes, heart attacks, and major surgery can worsen the symptoms. Here are the symptoms of vascular dementia.
- Having difficulties completing normal daily activities because of an inability to maintain concentration, communicate or follow instructions
- Problems with memory, though short-term memory is not affected
- During the night, there may be more confusion (called “sundown syndrome”)
- Sudden speech difficulties and sudden weakness can be stroke symptoms
- Personality changes
- Changes in mood, such as depression or irritability
- Changing walking speed, shuffling walking steps
- Balance and movement problems
- Urinary problems, including incontinence
- Tremors
Read: Transient Tic Disorder
How is vascular dementia diagnosed?
Your healthcare provider will order some of the following tests in addition to a medical history and physical examination:
- Computed tomography (CT): It is a type of imaging test used to make horizontal images (often referred to as slices) of the brain using X-rays and a computer. This type of image is more detailed than a regular X-ray.
- FDG-PET scan: A PET scan of the brain illuminates various regions of the brain with the help of a special tracer.
- Electroencephalogram (EEG): Measurement of brain electrical activity
- Magnetic resonance imaging (MRI): An imaging test using large magnets, radio frequencies, and a computer produces detailed images of the brain.
- Neuropsychological assessments: They can help distinguish vascular dementia from other types of dementia and Alzheimer’s disease.
- Neuropsychiatric evaluation: It might be done to rule out dementia or another psychiatric condition.
How is vascular dementia treated?
There’s no cure for Vascular dementia. Basically, we’re going to treat the conditions affecting blood flow to the brain. This can make the brain tissue less prone to further damage.
The following treatments may be used:
- Blood pressure, cholesterol, triglycerides, diabetes, and blood clot medicines.
- Make lifestyle changes like eating right, exercising, quitting smoking and drinking less alcohol.
- The carotid arteries, located in the neck and supplying blood from the heart to the brain, can be treated with angioplasty, stenting, as well as endarterectomy to enhance blood flow to the brain.
- Antidepressants are often prescribed for the treatment of depression or other symptoms, such as cholinesterase inhibitors for dementia.
Read: Stereotypic Movement Disorder
Living with vascular dementia
The progression of vascular dementia cannot be slowed, but the rate at which it advances can vary. The loss of mental and physical abilities might eventually require a high level of care for people with vascular dementia. An individual with disorder may not need hospital care until later in life if they have family members to care for them. It may become necessary to seek specialized care if the disease progresses.
A caregiver suffering from vascular dementia can receive some relief from the demands of caring for the demented individual through respite programs, adult daycare programs, and other resources.
Those affected by this type of dementia who cannot be cared for at home may be able to receive long-term care from facilities that specialize in caring for people suffering from dementia, Alzheimer’s, and similar conditions. If you require caregiver resources, you may check with your healthcare provider.
When should I contact my healthcare provider?
Talk to your healthcare provider about when to call those with vascular dementia. If you notice worsening symptoms (for example, obvious changes in your behavior, personality, memory, or speech) or if you notice new symptoms (such as sudden weakness or confusion), you should call your doctor.
Read: How to Avoid Alzheimer Disease
Prevention
There is a close link between the health of your brain’s blood vessels and the health of your heart. Your chances of developing vascular dementia may also be reduced if you follow these steps to keep your heart healthy:
- Be sure to maintain a healthy blood pressure. Both vascular dementia and Alzheimer’s disease may be prevented by maintaining a normal blood pressure.
- Control or prevent diabetes. Another way to reduce your risk of dementia is to prevent the onset of type 2 diabetes through diet and exercise. You may be able to prevent damage to your brain blood vessels by controlling your glucose levels if you already have diabetes.
- Don’t smoke. Every blood vessel in your body is damaged by smoking tobacco.
- Make sure you exercise regularly. Everyone should incorporate regular physical activity into their wellness plan. Exercise may reduce your risk of vascular dementia, among other benefits.
- Maintain a healthy cholesterol level. The combination of a healthy, low-fat diet and cholesterol-lowering medications, if needed, may reduce your risk of strokes and heart attacks. If you reduce plaque deposits inside the arteries of the brain, you may be able to avoid the development of vascular dementia.
A brief overview of vascular dementia
- The cause of Vascular dementia is lack of blood flow in the brain resulting in damaged brain tissue. The brain’s blood vessels can narrow or harden as a result of blood clots, ruptures, or narrowing.
- There are a lot of symptoms including memory problems, confusion, personality changes, loss of speech and language skills, and even physical symptoms like tremors or weakness.
- This typically worsens with time. A cure is not possible for Parkinson’s, but lifestyle changes and treatments for underlying causes (like high blood pressure, high cholesterol, diabetes, or blood clots) may slow its advancement.
- Blood flow improvements to the brain may also be beneficial. Dementia can be treated with other medicines, some of which may slow its progression or address symptoms it can cause.
- People with this disorder may have to go into long-term care or need full-time nursing care.